Allergies are one of the most common ailments seen by veterinarians in our patients. Pets often present itchy and uncomfortable with inflamed and irritated skin. Diagnosis and determination of the cause of the allergy can be very complicated, time consuming and frustrating. Allergies in our pets are generally due to food or environmental causes.
Atopic dermatitis, also known as an environmental allergy, is a common ailment seen by veterinarians in our patients. Atopic dermatitis has been defined as a genetic predisposition to inflamed and itchy allergic skin associated with the presence IgE antibodies directed against environmental allergens.
The skin is an important organ as it is in direct contact with the external environment and is the first line of defence against many pathogens. In the case of atopic dermatitis the exact mechanism of disease is not completely understood, but is thought to be either due to an immune system disorder manifesting in the skin or an abnormality in the skin barrier itself.
The diagnosis of atopic dermatitis can be more difficult, complicated, and time consuming than other diseases. This is due to the fact that the disease can present in many different ways. There are no classic clinical signs or a definitive test for the disease.
Diagnosis of the disease involves detailed patient history, physical examination, and ruling out of other causes of skin disease.
A list of 8 criteria has been formulated to assist in the diagnosis of atopic dermatitis has been developed and includes the following:
The presence of 5 of 8 of these criteria is sensitive for the presence of atopic dermatitis, but does not always allow us to distinguish between food and environmental causes of the skin disease. Depending on the specific allergen, atopic dermatitis can present either seasonally or non-seasonally. When symptoms are seasonal, it may increase a veterinarian’s suspicion, but is not confirmatory for atopic dermatitis.
It is essential to rule out other conditions that may present with similar clinical signs to atopic dermatitis. These include external parasites, microbial skin infections, food allergy, other skin diseases and neoplasia.
Allergy testing is not typically used in the diagnosis of atopic dermatitis. Allergy tests should only be used after a clinical diagnosis has been made based on patient history, clinical signs, and ruling out other causes of skin disease.
There is no single treatment that is “best” or “most effective” for pets diagnosed with atopic dermatitis. Atopic dermatitis is a complex disease with many different treatment options available. Treatment often involves a combination of several treatments to most effectively control your pets itching and inflammation. Your veterinarian will formulate a treatment plan that is tailored to your individual pet based on their clinical signs and response to therapy. Every patient responds differently to the various treatments and treatment combinations available. Therefore, treatment of canine atopic dermatitis can be complex and different approaches may need to be taken before one is identified that works best for your pet.
The main goals of treatment for atopic dermatitis are to reduce allergen exposure, treat and prevent secondary infections, reduce inflammation and itching, and to alter the immune response.
The main route of allergen exposure in atopic dermatitis is through contact with the skin. One of the main ways to reduce allergen exposure is through frequent bathing and rinsing. Your veterinarian may recommend a moisturizing or medicated shampoo to bathe your pet to reduce their exposure to allergens. The benefits of bathing are most likely due to the actual washing of the skin itself, rather than the medications in the shampoo. However, medicated shampoos may still be recommended, as they are helpful in treating and preventing any secondary skin infections. Bathing in cool or lukewarm water can also provide itching relief to your pet. Veterinarians usually recommend bathing your animal once weekly, and may recommend adding in a conditioner after shampooing if more frequent bathing is necessary or to prevent dry skin.
Your veterinarian may also recommend wiping or cleaning of your pet’s feet after exposure to allergens outdoors to decrease allergen exposure in between baths. Soaking your pet’s feet in warm Epsom salt baths may also be recommend to help decrease inflammation an itching.
Essential fatty acids have been shown to decrease inflammation and improve skin barrier function. Your veterinarian may recommend a new diet that this enriched with essential fatty acids or may supplement your pet’s current diet with an oral formulation of essential fatty acids. The benefits of essential fatty acids may take up to 6-8 weeks to be observed. Essential fatty acids are often ineffective as a sole therapy for pets with atopic dermatitis and are often used in combination with other treatments.
Antihistamines act by inhibiting the effects of histamine in the body. Histamine is involved in the body’s immune response and plays an important role in the production of itchy skin. Antihistamines are often ineffective as the sole therapy for pets with atopic dermatitis, but may be effective in pets with only mild symptoms. They are often used in combination with other therapies to address inflammation and itchiness. Some of the antihistamines that may be recommended by your veterinarian are diphenhydramine, certirizine, chlorpheniramine, and hydroxyzine. Each patient responds differently to different anti-histamines. Trials with more than one antihistamine may be necessary to determine which one your pet responds to best.
Corticosteroids, such as prednisone, prednisolone, methylprednisone, and dexamethasone, are very effective at rapidly reducing the inflammation and itchiness associated with atopic dermatitis. Treatment with corticosteroids usually starts at a higher dose to “put out the fire” of severe itching and inflammation. Then gradually over time, under the guidance of your veterinarian, the dose of corticosteroids is tapered to the lowest effective dose for your pet. The use of corticosteroids short-term generally results in side effects including increased drinking, urination, and appetite. Long-term use of corticosteroids can result in more serious side effects like dull and dry hair coat, weight gain, muscle wasting, panting, vomiting, diarrhea, elevated liver enzymes, and diabetes mellitus.
Corticosteroids are also available in topical spray formulations for treatment of localized areas of inflammation. Most topical corticosteroids are only used for 1-2 weeks, as long-term use can result in severe cutaneous damage.
Cyclosporine is an immunosuppressive drug that has been shown to result in a marked reduction in skin lesions and itchiness associated with atopic dermatitis. This drug is slower acting than corticosteroids and can take up to 4-6 weeks to take effect. Therefore, this drug is typically not recommended in managing flare ups of atopic dermatitis, but may be used in combination with other medications to provide relief. The most common side effects associated with cyclosporine include vomiting, diarrhea or soft stools, and gingival hyperplasia.
Oclacitinib is a novel treatment for atopic dermatitis and was recently licensed in Canada. Oclacitinib is an inhibitor of an important enzyme involved in the inflammatory pathway. Oclacitinib is effective at rapidly reducing the inflammation and itchiness associated with canine atopic dermatitis and can be used for managing flare-ups. The side effects associated with oclacitinib have been mild and have included mostly gastrointestinal upset, making this drug much safer than corticosteroids. Long-term administration of oclacitinib has been associated with increased susceptibility to infection but serious adverse side effects appear to be rare.
The main goals of allergy testing are to formulate allergen-specific immunotherapy and to identify allergens that can be avoided. Allergy testing is not used in the diagnosis of atopic dermatitis, but is typically considered after a clinical diagnosis has already been made.
There are two different tests that can be used for allergy testing. The first is a blood test that measures the levels of circulating allergen-specific IgE antibody to environmental allergens that are common to your area. The sample necessary for this test can typically be collected at your veterinarian’s office and sent off to a lab for analysis.
The second test is called an intradermal skin test. This involves injecting a small dose of several common allergens under the skin and looking raised and inflamed areas at the injection site. This test requires a lot of expertise and precision and is usually performed by a veterinary dermatologist.
Allergen-specific immunotherapy is one of the main goals of allergy testing. It involves gradually administering increasing quantities of an allergen extract to an allergic individual to help to improve the symptoms associated with subsequent exposure to the offending allergen.
Following identification of the allergens to which your pet is allergic, a specific allergen extract can be formulated. These allergen extracts can be prepared in injectable or oral/sublingual formulations. These allergen extracts will then be administered to your pet based on a schedule designed by you veterinarian. With ASIT therapy, improvements are observed gradually over time and it can generally take 6-9 months of therapy before improvement is observed. In terms of success of therapy, it is generally expected that 1/3 of patients on ASIT therapy do very well, 1/3 of patients improve sufficiently, and 1/3 of patients fail to improve. If ASIT is effective, it is usually administered for life. ASIT is the only treatment available that has the potential to bring about a cure or long-term remission of atopic dermatitis symptoms. The primary side effect of ASIT is increased itchiness as you are exposing the animal to the allergen to which it is allergic. Systemic and anaphylactic reactions are extremely rare.
A food allergy generally manifests as allergic skin disease or gastrointestinal symptoms, or both, that is triggered by food. In both dogs and cats, the most common food allergen is the protein content of their food, but other components of the food can also be the perpetrator.
A food allergy can develop in an animal at any age. A common misconception is that a change in diet triggers a food allergy. In reality, the body must have exposure to a protein before the immune system can react to it. Therefore, a food allergy can develop in our pets even if they have been on the same diet for their entire life.
The most common clinical sign observed in dogs and cats is non-seasonal itchiness. Cats classically have intense itchiness leading to self-trauma around the head and neck. In dogs, the itching is often mild to moderate in severity and itchiness and inflammation are typically most severe at the ears, feet, head, neck and the ventral abdomen. In other cases, food allergies can manifest as vomiting, diarrhea, or anal gland issues, with or without the skin lesions.
An elimination diet trial is the only way to determine if your pet has a food allergy. A diet trial involves an 8-12 week period during which only one food is fed. A diet trial must be very strict in that the pet cannot consume any other foods, treats, or supplements, aside from the prescribed diet.
After compiling a complete and detailed diet history, your veterinarian will help you select the appropriate diet to feed your pet during the diet trial. There are generally two types of diets that are recommended by veterinarians for diet trials. The first is a diet that contains a novel protein to which your pet has never been exposed to before. The second is a diet that contains hydrolyzed protein. Hydrolyzed proteins are proteins that have been chopped up into smaller pieces so that they are no longer recognizable by the immune system.
If your pet’s skin and/or gastrointestinal symptoms improve with the elimination diet trial, the diagnosis of a food allergy is then confirmed by a “re-challenge” test. The diet or ingredient that is suspected to be the cause of your pet’s allergies will be fed to your pet again. This will help to determine if your pet’s allergies were truly caused by the food or happened to resolve at the same time of the diet trial. A relapse of your pet’s symptoms can be seen anywhere from immediately to up to 14 days after starting the “re-challenge” test. If a relapse in symptoms occurs, then a food allergy is confirmed.
The best diet for ongoing treatment of food allergy is a diet that does not contain the allergen to which your pet is allergic. For your pet, this may mean to continue on the diet used in the elimination diet trial or to find another diet that does not contain the ingredient to which your pet is allergic.
The pancreas is an organ that produces digestive enzymes as well as hormones require for glucose control in the body. The three hormones required for glucose control are insulin, glucagon and somatostatin. Insulin is secreted in response to high blood glucose levels in the body. Ultimately the insulin helps to lower the blood glucose by increasing the uptake of glucose into the cells and storing the excessive glucose as glycogen in the liver for later use. It is also responsible for breaking down fat and storing it as adipose tissue. Glucagon is secreted in response to low blood glucose levels. It helps to raise the blood glucose by converting the stored glycogen in the liver back to glucose. Somatostatin helps to regulate blood glucose levels in conjunction with insulin and glucagon as well as helps to decrease gut motility and secretion of digestive juices.
Damage to the pancreas can occur secondary to eating poor quality foods, table scraps and when chronic gastro-intestinal disorders such as inflammatory bowel disease occur. When the cells of the pancreas are damaged insulin secretions will decrease and glucagon blood levels will increase. The lack of insulin in the body, along with the rising levels of glucagon, results in high blood glucose (hyperglycemia) for an extended period of time.
When blood glucose levels rise above 10-12 mmol/L in dogs and above 12-15 mmol/L in cats, the kidneys are no longer able to resorb all the glucose, which results in glucose spilling into the urine. Glucose is therefore detectable on a urine test strip. The loss of glucose in the urine leads to an increase in urine production, increase in thirst, and dehydration.
The chronic high glucose levels will lead to tissue injury of the blood vessels, which causes the blood vessels not to function normally. The exact mechanism of why this occurs is not fully understood. When the blood vessels fail to function normally, it leads to inadequate blood supply to the tissues. As the blood sugar increases, a pet can experience one of two types of emergencies: diabetic ketoacidosis (DKA) or hyperosmolar hyperglycemic state (HHS).
Because there is a lack of insulin in the body, the body shifts from carbohydrate metabolism to fat metabolism. As the fat is metabolized for energy, it produces acidosis; coma or death may occur. Pets with DKA often present with symptoms including polyuria, polydipsia, nausea, weakness, vomiting and diarrhea. Other signs may include shock, panting, cold body, hypotension and dehydration. Approximately 40% of dogs may present with cataracts in one or both eyes. Enlarged liver and secondary pancreatitis are common in both the dog and cat.
It’s not fully understood why the pet does not experience ketonuria since the pathogenesis is similar to that of an uncomplicated diabetic. It is thought that there are likely some functioning cells that are still producing some insulin for the pet. The existence of some insulin prevents the formation of ketones. As the blood sugar level increases, the pet begins to experience severe signs of dehydration. Pets with HHS are often lethargic, severely dehydrated, depressed and weak. They may have gastrointestinal signs (anorexia, vomiting, diarrhea), which may progress to neurological symptoms. They are often in shock and hypothermic. As the condition progresses, the pet may experience a coma and/or die.
Diagnosis is made based on laboratory findings. A complete blood count (CBC), blood chemistry, electrolytes, urinalysis (sterile sample ideal) and blood gas should be performed. In both the dog and cat, a mild polycythemia (due to dehydration) or leukocytosis may be noted.
A biochemistry panel may reveal increased liver values, most commonly ALT and ALP. Increases in blood glucose, kidney enzymes and cholesterol are often noted. A urinalysis reveals glucosuria and, most likely, in the case of DKA, ketonuria. Protein, bacteria (due to secondary urinary tract infection) and/or blood may also be present in the urine.
Hypoglycemia is one of the most common side effects of insulin therapy in a diabetic. Clinical hypoglycemic is defined as blood glucose levels less than 4 mmol/L. Diabetics who experience a hypoglycemic state do so because of one of two reasons: they were incorrectly dosed with insulin or are experiencing a change in insulin requirements. Cats frequently can experience “transient diabetes” causing their insulin requirements to change. Approximately 20% of diabetic cats will experience transient diabetes. Changes in the pet’s weight, appetite, diet, and activity level can result in the pet needing a lower insulin dose. Owners of new diabetics should be given written instructions on ways to avoid hypoglycemic episodes (give insulin after ensuring pet has eaten, have family member double check dose, keep a check system on the refrigerator).
Hypoglycemia mainly affects the nervous and musculoskeletal systems. Nervous tissue relies heavily on glucose as its primary energy source. While emergency signs resulting from hyperglycemia take days if not weeks to occur, a pet experiencing hypoglycemia is always an immediate emergency. Pets who experience hypoglycemia will often become lethargic, weak, ataxic and appear “wobbly.” Signs can be seen when blood glucose is between 2-3 mmol/L. Hypoglycemia stimulates appetite, so pets may start acting hungry or eat things they normally may not. As the hypoglycemia worsens (the blood sugar level continues to decline), the symptoms will worsen and can lead to seizures, coma and death. Patients with a blood glucose between 2-4 should be offered a meal (canned food). If they will not eat they should be given some corn syrup (1-2 teaspoons) in the mouth. The blood glucose should be checked in 15-30 minutes to see if the glucose is going up. If it continues to drop the patient should be taken to the veterinarian. If the blood glucose goes up and the patient is behaving normally check the blood glucose again in 30 minutes and then every 2 hours thereafter to ensure that the blood glucose remains stable. You should call your veterinarian to discuss the problem and what to do about the next scheduled insulin injection.
Upon presentation of any emergency diabetic, all critical signs should be treated. Patients may present severely lethargic, in shock, obtunded, seizing or in a coma. All known diabetics should immediately have their blood glucose level tested to ensure the signs are not from hypoglycemia. Hospitalization and supportive care will be instituted to help and correct electrolyte imbalances, and normalizes the blood glucose levels and treat for any other illness, such as pancreatitis. After the patient is stable home care will be started using insulin by injection. Dietary recommendations and an exercise problem will also be advised based on the patient’s specific needs. We do not expect blood glucose to be normalized overnight and in cases where underlying diseases such as urinary tract infection, dental disease, Cushing’s disease and pancreatitis it may take some time for control to be appreciated. In some patients treatment of underlying disease, such as dental surgery may be needed before diabetes is controlled.
Insulin injections should cause lowering of the blood glucose. The number one rule about insulin injection is that if you are not sure if you have given the injection properly or you feel that some did not go into the skin DO NOT give a second dose. Giving a second dose of insulin could cause a hypoglycemia. Remember it is safer to have elevated blood glucose compared with low blood glucose. You will know when the insulin is starting to work and diabetes is becoming controlled because the increased drinking and urinating will start to normalize.
All insulin should be stored in the refrigerator between uses. If left out for less than 24 hours the insulin will be safe and effective for continued use. Insulin should be gently agitated when ready to use to ensure that all aspects of the insulin are mixed together. This is especially important with Caninsulin. Caninsulin must have the specific caninsulin syringes for administration. These can only be purchased at the veterinarian and are not available or the same dosing as the insulin syringes found the drug store. Glargine insulin can be injected using ½ cc 100 unit insulin needles found at the drug store.
Caninsulin for dogs, and Lantus (glargine) for cats are the two insulin products of choice at Avonlea and Hollybank. The different types of insulin have different characteristics which will affect how fast and long they affect blood glucose. The insulin dose and frequency will be dependant on how the dog or cat responds to the insulin. Blood glucose levels are required to help to determine the amount of insulin as well as the dosing frequency. The insulin dose should not be changed unless a glucose curve has been performed. Generally speaking all patients will start on once a day injection and if necessary, based on the glucose curve, every 12 hours dosing will be recommended. Your veterinarian will advise on any dose changes.
It will be your job to check your dog or cats blood glucose level at home. This is a much less stressful process compared with having the veterinarian perform the tests. It also allows you to have the ability to troubleshoot your pet’s glucose level if things don’t seem right. You will need to purchase a “one touch glucometer” with about 25-50 test strips. This particular glucometer is very simple to use and does not require calibration. If you have a glucometer it is fine to use. There is not specific pet versus human glucometer. On cats blood is collected from the lateral ear margin after nicking the ear with a needle. Only one drop of blood is needed. A good range for blood glucose control in a cat is between 5-12mmol/L. In dogs blood can be collected from the ear or from the inside of the lip. Again only one drop of blood is needed. A good range for blood glucose control in a dog is between 5-9 mmol/L. Dogs require more stringent control of the blood glucose as they are very prone to developing ocular cataracts with uncontrolled diabetes.
Newly diagnosed diabetics should have their blood glucose checked at different times of the day during the first week of insulin therapy to help and get you and your pet used to the process. The most common problem that occurs with collecting the blood is that a large enough drop is not present to assess the blood with the glucometer. If you get “error” on the glucometer you likely do not have enough blood. When this occurs simply scrape the wound or make a new wound for the blood collection.
When performing a blood glucose curve you will need to collect blood every 2 hours in dogs and every 4 hours in cats. The first blood collection is at the time that insulin is given. This is considered to be time 0. So for a dog blood will be collected at time 0 then every 2 hours afterwards until 8 readings have been collected. This would be a total of 16 hours. For a cat blood is collected at time 0 (time of first insulin injection) then every 4 hours after the insulin injection, for 4 collections. This is a total of 16 hours. When submitting the glucose curve you must indicate how much insulin was given, the time of the injection and how much and the type of food that was fed as well as if any exercise was performed during the time of the curve. Your veterinarian will review the curve and advise on any insulin, dietary and exercise changes as required.
Glucose present in the urine is a sure sign that diabetes is not under control. Human urine test strips can be purchased from the pharmacy and be used throughout the day to help and determine if your pet’s diabetes is under control. These are most beneficial for use after diabetes is controlled. When diabetes is controlled the increased drinking and urination will subside. If your pet has been well controlled and you notice increased drinking and urinating and you are not a fan of doing the blood glucose collection you can check the urine glucose first and if glucose is present in the urine you will then be justified in performing a glucose curve. Insulin levels should not be changed based on urine glucose levels.
Cats require a high protein and low starch (carbohydrate) diet to help control blood glucose levels. Many cats show excellent diabetes control when using canned food and minimal dry food. Some cats will even revert to a non-diabetic status with minimal time using insulin injection. A prescription diabetic food should be fed at specific quantities divided into 2 or 3 feedings per day.
Dogs generally require a high fibre low fat diet to help with diabetic control. Fibre will slow down emptying of food from the stomach, and will slow down the digestion of carbohydrates (glucose sources). This means that blood sugar levels will not jump as high after eating compared with that of patients fed low fibre diets. Because many diabetic dogs also suffer from pancreatitis food recommendation will also be low in fat content. Fat will stimulate the pancreas to activate which can cause inflammation, vomiting and pain, all of which will interfere with diabetic control.
Your pet’s kidneys filter and remove waste from the blood stream. The term kidney failure, kidney disease, renal disease, or renal insufficiency are all interchangeable terms that mean that the kidneys are not able to do at least some of the tasks they are supposed to do as well as they are supposed to do them. Kidney disease can affect any pet but is most common in older pets, being one of the leading causes of mortality in senior cats. Often signs of kidney disease are not seen until over 2/3rds of the kidney function is lost. The good news is that kidney disease is one of those conditions where early intervention can make a big difference and normal life quality can be maintained for sometime, even years depending on the individual.
Common symptoms of kidney disease that you may have noticed in your pet include:
The diagnosis of kidneys disease is made from blood and urine tests which determine how well your pet’s kidneys are functioning and the best treatment for your pet. To fully understand the consequences of kidney disease and the treatment for it we first need to understand the full functions of the kidney.
Before reviewing what failing kidneys can no longer do, it is important to know what normal kidneys do. Kidney function goes far beyond just making urine. Kidneys are made of millions of processing units called nephrons. These tiny processing units are responsible for separating the chemicals you want to keep in your body from the chemicals your body needs to dispose of. Once a nephron is destroyed by a disease, it cannot regenerate; this means that we all have a finite number of nephrons to last us our whole lives. Fortunately, we have many extra nephrons, so many extra that overall kidney function does not fall behind until we are down to about 1/6 of our original number of nephrons.
The chemicals the kidneys remove are dissolved in water and make up the fluid we all know as urine. Here is what your kidneys do for you and your pet, what they become unable to do in renal insufficient, and some of the parameters we track:
Hydration of the body depends on both water consumed and water removed or excreted. When the body is dehydration, the kidney must respond by conserving water. This means that all the chemicals that the body needs to get rid of still need to removed, but the kidney needs to manage this using the smallest amount of water possible. Similarly, if you drink too much water, the kidney needs to efficiently remove the excess water to prevent dilution of the blood stream. A pet with decreased kidney function will not be able to make concentrated urine and will need to drink extra water to process the body’s waste chemicals. For this reason, excessive water consumption is an important early warning sign and should always be investigated.
When we analyze a urine sample, one of the most important parameters is the urine specific gravity. This is a measure of how concentrated a urine sample is. Water has a specific gravity of 1.000. A dilute urine sample has a specific gravity less that 1.025 in dogs and less than 1.030 in cats. A concentrated urine sample would have a specific gravity over 1.025 or 1.035 respectively. A failing or diseased kidney cannot make concentrated urine; the patient must drink excessively to get enough water to excrete the toxic chemicals load. As kidney disease progresses, the animal cannot drink enough and toxic chemical levels begin to rise in their body. Weight loss, listlessness, nausea, constipation, and poor appetite become noticeable.
The kidneys remove our metabolic waste for us. If there is inadequate circulation going through the kidneys or if there are not enough functioning nephrons to handle the waste load, toxins will build up. When they build up and exceed the normal range, a condition called azotemia exists. If the toxins build up to a level where the patient actually feels sick, a condition called uremia exists. If we can keep our azotemic patient below the uremic level, they feel fairly normal and have good life quality.
The most important marker of uremia is called creatinine, which is a by-product of muscle break-down and is normal in the bloodstream in small amounts. The kidney is responsible for removing this molecule and measuring the amount of this molecule in the bloodstream is an important indicator of kidney function. A newer parameter called SDMA (symmetrical dimethylarginine) becomes abnormal much earlier than creatinine and is becoming more commonly tracked. We stage or rate a pet’s kidney disease based on creatinine blood level and SDMA level (see the staging section below). Another marker is BUN, which stands for blood urea nitrogen. This parameter is similar to creatinine but is influenced by more dietary protein as well as kidney function. These three markers are central to determining the severity of a kidney problem.
The balance between calcium and phosphorus in the blood is important. Too much of one or the other will lead to crystals forming in the tissues of the body and weakening of the bones to the extent they may actually become rubbery. The kidney plays an important role in this balance and when kidney function is lost, phosphorus levels begin to rise. Therapy for insufficiency kidney function requires monitoring of phosphorus levels and the use of diet and medications to keep phosphorus levels in a reasonable range.
The kidney plays a major role in controlling electrolyte balance as well. In particular, conservation of potassium is an important aspect. Insufficient kidneys lose their ability to conserve potassium and potassium levels begin to drop leading to weakness. Potassium supplements are commonly needed in the treatment of kidney failure.
Blood pressure sensors in the kidney help regulate blood pressure in the body. When these are damaged, hypertension (high blood pressure) can result and can damage the kidney further. Blood pressure is commonly measured in kidney failure patients. Hypertension (increased blood pressure) is especially common in patients that are losing protein in their urine.
There are a lot of important proteins circulating in the bloodstream and it is crucial that they are not lost in urine. The nephron possesses a complex filtration system that keeps protein in while removing harmful wastes. If the nephron’s filtration system is damaged (in what is known as glomerular disease), a much more severe form of kidney failure results. Screening for this damage is an important aspect of staging kidney failure and a test called a urine protein:creatinine ratio is often included in the testing profile to assess this condition.
The kidney produces a hormone called erythropoietin. This hormone signals the bone marrow to make more red blood cells. In the absence of this hormone, a non-responsive anemia occurs and can get so bad that transfusion is necessary. Erythropoietin can be given by injection to alleviate this problem but there are some potential pitfalls in doing this. Hematocrit and PCV (packed cell volume) are measures of red blood cell volume that are commonly monitored in kidney patients.
Metabolic processes require a narrow pH range for efficiency. The kidney also regulates this balance and if it cannot, intervention is necessary, usually in the form of fluid therapy.
Pets, like humans, are normally born with two kidneys and lots of extra nephrons. Over time these excess nephrons are destroyed, secondary to disease or age. When your pet is down to less than one-third of their kidney’s worth of nephrons, test results become notably abnormal and it becomes important to make lifestyle changes for your pet. How big these changes are depends on how far things have gone out of whack when the problem is discovered. Early detection of poor kidney function is one of the main reasons laboratory screening tests are recommended.
Staging
The International Renal Interest Society (IRIS) has posed the following staging criteria for pets with Stage I being pets with evidence of kidney disease but no evidence of a change in actual kidney function, all the way up to Stage IV where pets feel sick from their disease. These stages are based on blood creatinine levels measured in umol/L. It is worth noting that MANY patients are well past IRIS Stage IV at the time of diagnosis, making the IRIS Stages best for characterizing the earlier stages of renal insufficiency. For patients in more dire initial states, the goal is to drive their toxin levels down to where the IRIS system becomes relevant.
|
There is no set time frame for progression through the stages of renal disease. Some pets can remain in the early stages of renal disease for many years before progressing while others will worsen in months time. Monitoring is required to ensure your pet is getting the support they need for each stage of this disease.
A Note on Pyelonephritis and Infection
Pyelonephritis is another name for kidney inflammation and usually means kidney infection. Pets get kidney infections when a bladder infection goes unnoticed or incompletely treated long enough and the bacteria go up the ureters into the kidney where they set up shop and cause damage and pain. This form of kidney failure has the most potential for reversal or partial reversal, making it important to culture the urine early. A simple urinalysis is frequently unable to detect infection in this situation as the pet drinks so much water that the visible markers of infection are diluted out and cannot be found.
There is a wide range of what is involved when a patient has kidney failure or insufficient kidneys. Each pet will have a different stage and a different constellation of issues to contend with. Some will need only a diet change and some will need on-going fluid therapy at home or hospitalization. Prognosis depends on all the factors involved. Your veterinarian will let you know what your particular pet needs and will be watching many different lab tests to keep control of your pet’s condition.
What signs will I see if my pet has kidney disease? How do I know if the disease is progressing?
You should monitor for an increase in drinking, urination, decreased energy or appetite and for vomiting, diarrhea and weight loss. If your pet is showing a sudden change in appetite or behaviour your pet should be seen as soon as possible by your veterinarian. Worsening clinical signs does not always mean your pet’s chronic disease is worsening, as pets with kidney disease are more prone to kidneys infections which can make the kidneys work harder. Early treatment can lead to prevention of further damage to your pet’s kidneys and a better quality of life.
Increase Water Intake
Your pet will be drinking and urinating more frequently. It is important to always have fresh water available and to try to increase the amount of water your pet is taking in. As kidneys lose their ability to concentrate urine the fluid that they drink goes right through them, leading to an increased risk of dehydration. Feeding a canned diet and increasing water bowls in the house can help your pet to stay hydrated.
Dietary Therapy of Renal Failure
Many aspects of kidney failure require attention. Diet can be used to help in many ways and we are lucky to have commercially available diets made specifically for renal patients. There are even diets made for different stages of kidney failure. The goal of therapy, dietary or otherwise, is to prevent or at least postpone advanced uremia (poisoning by toxins that the kidneys could not adequately remove) and extend life expectancy.
In one famous study where 38 dogs in kidney failure were tracked for 2 years, dietary therapy reduced the risk of dying by 69% over dogs allowed to continue eating regular dog food.
Another study in dogs showed that beginning the renal diet when the creatinine was between 2.0 and 3.1 delayed the onset of uremic crisis by 5 months.
A recent study involved 50 cats with stable, naturally occurring renal failure that were divided into two groups, one receiving a renal diet and the other receiving regular food. The cats on the renal diet survived over twice as long as the others.
There is tremendous benefit to your pet in switching to a therapeutic renal diet. Unfortunately, renal patients tend to be very picky and the diets are not always acceptable to the pet. To aide in the transition to your new renal diet your pet should be very gradually transitioned to their new food, over 7 to 10 days, starting with no more than 25% of a new diet. Often renal patients will become picky and rotating through a number of different renal diets will help to maintain your pet’s appetite.
Let’s review some basic features of a desired diet. There are many misconceptions about an appropriate diet for renal disease. The ideal food for your pet depends on their stage of renal disease. Some basic desired qualities in a renal diet are:
Low Protein
As a number of renal toxins come from the metabolism of protein, one way to give the kidneys less work to do is to feed a diet lower in protein. How much less protein depends on how serious the kidney disease is. Older animals tend to require a higher dietary protein level in general when compared to their younger counterparts. Protein also adds palatability to the food so that if we try to restrict protein too much we may end up with a pet who will not eat at all.
Further, there is a metabolic requirement for protein below which a diet cannot dip. This has led to diets with differing protein restrictions to fit with different stages of disease, less restriction for earlier stages.
Phosphorus Restriction
This is an important part of a renal diet since phosphorus balance is crucial. Phosphorus comes into the body via the diet and leaves the body via the kidney, only in renal failure phosphorus is not well removed as it is supposed to. Using less phosphorus in the diet may be adequate to keep the blood phosphorus levels normal, thus balancing the intake with the output, but sometimes addition of medication (i.e. a phosphate binder) is needed to further reduce intake. Restricting dietary phosphate has been shown to slow the progression of renal disease.
Omega 3 Fatty Acids
Studies suggest that kidney failure patients taking omega 3 fatty acids are likely to live longer than patients who do not take them. This has led to the supplementation of most renal diets with fish oils. The full import of fatty acid supplementation is still being worked out.
Other dietary features include B vitamin supplementation (since the damaged kidneys tend to lose excess B complex), which have non-acidifying features to help control acidosis.
At What Point Should a Special Diet be Started?
This question has been controversial for a long time. For many animals, changing diet to a less palatable food represents a definite reduction in life quality. There was some thinking that we are changing the diet too soon. On the other hand, if a pet is in a more advanced state of disease before the switch is made, the pet will be much less willing to change to a food of less palatability. The companies that make these foods have put a great deal of research into improving palatability over the years, which has helped tremendously.
Now the International Renal Interest Society finally has guidelines. They recommend changing the diet to a renal food when a dog’s creatinine level is in the Stage III renal failure. For cats, the diet should change when the creatinine reaches approximately middle Stage II renal failure).
These guidelines allow the patient to benefit the most from the preventive advantages of the diet. If the pet finds the diet palatable, then there should be no life quality issues with changing foods.
Home Cooking a Renal Diet
Home cooking an appropriate renal diet is a complicated task but it can be done. Because different pets experience different problems with their renal disease (potassium depletion or not, pH issues or not, different degrees of phosphorus restriction needed, etc.), the diet should ideally be tailored to the individual. If you would like to home cook for your pet please contact us to discuss appropriate recipes that are available.
Subcutaneous Fluids at Home (cats)
Chronic kidney disease patients in the later stages of their disease may require extra fluids beyond what they drink to wash dangerous renal toxins through their systems. Subcutaneous fluids, especially in the treatment of advanced chronic renal disease in cats, can aide in the quality of life of your pet. Although your pet is drinking frequently, most of the water is excreted through their kidneys, with little being available to their bodies. Subcutaneous fluids help to keep your pet hydrated and helps your kidneys to flush some the toxins from their system.
Although giving subcutaneous fluids at home can sound daunting, it is often better accepted and easier than giving your pet a pill. If subcutaneous fluids are recommended for your pet we will start by giving you an in clinic tutorial with your pet to ensure you are comfortable with this at home.
Antacids:
One of the effects of toxins (including creatinine and urea) building up in your pet’s bloodstream is gastrointestinal inflammation. Starting an Antacid such a Ranitidine or Pepcid can help to minimize this inflammation and aide in your pet’s appetite. Antacids are available as both a pill and as an injection, with often the injectable being very well tolerated in most pets.
Additional Medications:
There are a variety of additional medications that may be recommended for your pet to help support their quality of life and help to minimize the progression of their renal disease. A few of these include:
Please do not hesitate to contact us if you have any questions in regards to treatment of your pet’s Chronic Renal Disease.
Chronic Renal disease is a common occurrence in pets today. With early recognition of signs and diagnosis your pet can maintain a good quality of life and possibly slow the progression of the disease. In late stage renal disease there are numerous therapies available to help maintain your pet’s quality of life.
Please do not hesitate to contact us to discuss your pet’s kidney disease if you have any additional questions or would like to discuss your pet’s individualized treatment plan.
Our pets’ ability to get around is very important but can be easily taken for granted, until something changes. Getting to the litterbox or outside to toilet, playing and going for walks, even climbing up on the bed or couch to snuggle, are important parts of our pets’ life with us. When an injury or illness affects your pet’s mobility, it can be difficult to adjust. But don’t worry, even if the cause of the problem can’t be reversed, there are lots of ways to help maximize your pet’s remaining ability.
Sometimes the signs are obvious such as suddenly being unable to walk normally. However, other times there could be a gradual subtle onset of the signs. Here are some examples of signs that could indicate a mobility problem and should be brought to your veterinarian’s attention:
The definitive treatments your pet needs will depend upon the diagnosis, so most of this discussion will focus on things that can help your pet in general with a chronic mobility impairment.
Medication may be needed for pain relief or to help decrease inflammation. Other medications may be needed depending on the type of problem.
Surgery may be required for a torn ligament, fracture, dislocation, or intervertebral disc disease.
Small dogs and cats can be carried and their weight can be supported by hand. Larger dogs may benefit from a towel under the belly as a sling or a special harness to assist lifting and supporting their weight. Dog and cat wheelchair carts can be purchased for patients with hindlimb paralysis. Litterboxes with low sides can be provided in a location that is easy to access, or a ‘potty patch’ indoor toileting spot can be provided for a dog.
The saying ‘if you don’t use it, you lose it’ is very true for mobility. Regardless of the cause of the mobility impairment, there are simple movements and types of exercise that can help increase functionality and strength in the affected limb. Your veterinarian will explain the type of exercise that is best for your pet, as well as simple movements your pet can learn to do to stretch or strengthen specific areas of the body that require it. There are even veterinarians with advanced training who specialize in this type of care (similar to a human physiotherapist).
Some examples of pet physical therapy are: sit-stand repeats (‘doggy squats’), walking up/down stairs or ramps, walking over obstacles or through water/sand, swimming, having your cat reach for a dangling toy, stretching major muscle groups, massage.
Pets who will be spending more time lying down will need thick soft bedding. If unable to turn themselves, they will need to be turned from side to side every few hours. This is very important in preventing bedsores and calluses.
Cats and dogs who can’t get around easily still need to be part of the family and engage in things they used to enjoy as much as possible. This is where you can really make a difference in your pet’s life. Steps can be placed to help a cat climb up to their favourite spot by the window to watch the birds. A dog’s bed can be moved into the living room to spend more time around the family activities. A cat can still be encouraged to play by using a different type of toy. If a dog can no longer romp in the park and catch a Frisbee, he may still enjoy cuddling by the fireside with you.
Osteoarthritis is a chronic degenerative disease that may affect any joint but commonly affects your pet’s hips, elbows, stifle (knee), carpus (wrist) or intervertebral joints (in the spine). It is the first cause of chronic discomfort in pets. It occurs when cartilage in the joint is damaged, either following a traumatic event, due to constant minor traumas such as the wear and tear associated with athletic animals, obesity, or abnormal joint formation.
Cartilage reduces joint stress by cushioning the ends of the bones, like a shock absorber. When cartilage is damaged, a cascade of inflammatory changes occur, leading to the destruction of the cartilage and damage to the underlying bone. Cartilage has no nerves, so if your pet is showing signs of pain, the damage to the underlying bone has already begun.
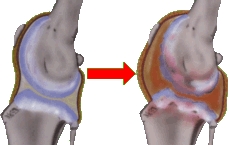
Osteoarthritis
Osteoarthritis is very common, over 45% of dogs above the age of 8, and 90% of cats over the age of 12 have osteoarthritis.
Dogs:
Cats:
*Notice that for both dogs and cats, whimpering, yelping, crying out or other vocalizations are not a common sign of arthritis pain. Just because your pet is not saying anything out loud, does not mean he or she is not in pain! Look at what she or he is saying without words.
Usually a veterinarian will suspect osteoarthritis based on your description of your pet’s signs, along with having risk factors such as old age, previous joint injury or surgery etc. An orthopedic examination and gait analysis will usually be performed to help localize the joint(s) that may be involved and gauge the severity. Xrays (radiographs) may also be required to rule out other causes for your pet’s pain or mobility changes, as well as to look for arthritic changes in the joints.
There are many things that can be done to help with your pet’s osteoarthritis; it does not have to be accepted as an inevitable part of aging! True, the underlying degenerative process cannot be completely reversed, but depending on your pet’s needs, any or all of the following treatment and management strategies can help (there is more information about each one outlined below):
Studies have shown that an 11-18% weight loss has the same effect on joints as daily supplements. The extra weight places excessive pressure on joints, leading to further deterioration. Please speak to us about a weight loss plan if your pet is overweight.
These are all geared towards helping to provide your pet’s body with building blocks to repair cartilage and improve the quality of the joint fluid, reduce inflammation and slow the degenerative process. If started when osteoarthritis is in early stages, these can be very helpful.
Contains Green-lipped Mussel Powder, which includes glucosaminoglycans and omega 3 fatty acids to support joint health. Also designed for the best nutrition of older pets.
Green-Lipped Mussel Powder to be added to your pet’s food.
A tasty chew to help your pet’s joints. Includes:
Devils Claw (Harpagophytum Procumbens) has traditionally been used to relieve pain associated with arthritis; it’s pain relieving properties have been studied as comparable to some NSAIDs. Very safe with minimal side effects.
Omega 3 fatty acids and Vitamin E: have been shown to have marked anti-inflammatory effect when added to the diet at appropriate levels.
Chondroitin and Glucosamine: The building blocks for cartilage.
The same as Flexadin Plus but instead of Devil’s Claw, it contains undenatured collagen type 11, another joint building block.
The saying, ‘if you don’t use it you lose it’, is very true of bones, joints and muscles.
Physical therapy may sound complicated, but it can be as simple as taking your dog for a walk, or playing with your cat. Joints need to move and bend to reduce stiffness, and to move joint fluid around them to lubricate all areas of the joint. Muscles weaken if not used (if your pet is favouring a limb or is less active), and this weakness will only serve to worsen their mobility difficulties.
Your veterinarian will explain the type of exercise that is best for your pet, as well as simple movements your pet can learn to do to stretch or strengthen specific areas of the body that require it. There are even veterinarians with advanced training who specialize in this type of care (similar to a human physiotherapist).
Some examples of pet physical therapy are: sit-stand repeats (‘doggy squats’), walking up/down stairs or ramps, walking over obstacles or through water/sand, swimming, having your cat reach for a dangling toy, stretching major muscle groups, massage.
An injectable, plant-source, ‘disease modifying agent’ that is used to target and improve the degenerative process in the joints by providing building blocks for repair as well as turning on joint repair processes. A simple injection under the skin, this can be given by the veterinarian or you can even learn how to do this at home for your pet.
NSAIDS
Some commonly used brands are Metacam and Rimadyl. These are medications specifically for pets that decrease inflammation and pain in the joints. NSAIDs are very helpful and effective for arthritis. They may not be an option for every pet due to other health problems they may have or possible side effects.
Additional Pain Medications
Commonly used additional pain medications include: Tramadol, Gabapentin, Buprenorphine. These medications reduce pain and can be used along with NSAIDs if needed, or on their own for pets who should not be given NSAIDs.
Aging is a fact of life for us all. Physiologically, aging is a process of gradual breaking down of the normal function of each body tissue and organ. This can occur more rapidly or more slowly in different species, breeds, and different individuals. There are many normal aging changes, but there are also illnesses that can with age. There are things that can be done to detect and treat these problems as well as to help maintain vitality even with normal aging changes. Your pet’s senior years can be a wonderful time for you both to enjoy in giving and receiving different things from when your pet was younger. Your pet may need more help with grooming, mobility, and medications, but will give back with quiet moments together and a deep knowledge of and trust in each other from years of bonding.
Most pet owners wonder ‘how long will my pet live?’ Though no-one can say for sure, the average lifespan of pets with the good medical care that is available to us today, is:
Cats: 15-17yrs
Small & medium dogs: 14-16 yrs
Large dogs: 12-14 yrs
Giant dogs: 9-10 yrs
Some changes are to be expected as your pet ages, however other changes can signal a disease that may need treatment. Some age-related conditions that commonly affect humans like arteriosclerosis (hardening of the arteries), heart attacks, or osteoporosis (weak/brittle bones) are rare in dogs and cats.
Weight – A very slow gradual loss of muscle mass is normal. A good senior diet should help to maintain muscle mass for your senior pet. More rapid changes in weight up or down (over 6 months or less) should earn a visit to the veterinarian.
Sleep – Sleeping more is normal, and seniors often sleep deeper and may have more noticeable dreams (with more vocalizations or body movements). However, changes in sleep patterns such as a dog being awake at night and sleeping during the day may signify a problem.
Hearing – Gradual onset deafness can be normal and will often affect either high or low tones first before gradually progressing to complete deafness. Sudden deafness may be due to an ear problem and should be looked into.
Vision – Slightly bluish or cloudy lenses (‘lenticular sclerosis’) is normal but should not significantly affect your pet’s vision – difficulty seeing or cloudy eyes should always be evaluated by a veterinarian as there are several causes and this can often be treated to save your pet’s vision.
Lumps – Lumps do occur more commonly as pets age, and there are several types that are benign, however, every lump should be carefully checked to ensure proper treatment is performed if it is a concern. Many benign lumps are identifiable on sight, but your veterinarian may recommend a needle sample or biopsy of a lump to investigate what a particular lump is.
Playfulness – A gradual decrease in play can be normal, however your senior pet should still show interest in things they used to enjoy, even if they are not as bouncy or spend less time playing. A lack of interest in your pet’s usual favourite things is usually a sign that they are not feeling well.
Activity and Slowing Down – Activity level will generally decrease gradually, however, this can also be a subtle sign indicating that your pet doesn’t feel as good as they should, due to arthritis or other illnesses. Never ignore this sign, especially if it is a more sudden change, or your pet is showing other changes along with it. Increased activity especially pacing or walking in circles should also be discussed with your veterinarian.
Mobility – Stiffness, difficulty rising or jumping, and other mobility changes are not just something to accept as a part of aging. Arthritis is very common in seniors but it is a health problem and there are treatments available to help your pet feel and move better.
Appetite and Eating Habits – Decreased appetite and decreased food intake is always a concern, this is never normal. A noticeable increase in appetite can also be seen with a few different health problems for both cats and dogs. Vomiting is never normal aside from a hairball every few months in cats.
Teeth – Over time, tartar will accumulate and gum disease will set in, however this is not something to accept as normal. Tartar buildup, inflamed gums, bad breath, loose or missing teeth or growths in the mouth are all health concerns. Don’t wait – have your pet’s dental health addressed before he or she gets older or the problem gets worse.
Drinking – Your pet’s water intake should stay the same throughout their adult life. An increase in water intake (needing to fill the bowl more often, seeing your pet drinking more often or for longer periods of time) can definitely be a sign of a health problem.
Toileting – Toileting problems are never normal for dogs or cats. Increased urine frequency or amount, constipation (no stool for 2 days in dogs or 3 days in cats), incontinence, inappropriate elimination (urine or stool indoors for dogs or outside of the litterbox for cats), straining to urinate or defecate, diarrhea are all examples of abnormal toileting habits that should warrant a veterinarian visit.
Behaviour – No behaviour changes are normal or expected with aging. Unusual aggression or grumpiness can be due to unnoticed vision or hearing loss, pain or other health issues. Brain aging and cognitive dysfunction (dementia) can look like a loss of house or litterbox training, staring into space, pacing or circling, forgetting usual routines or getting lost in the house, unexplained anxiety, or a loss of recognition of family members. There is help for this.
Any health or behaviour changes that you feel are abnormal for your pet are worth bringing to the attention of your veterinarian. Some diseases such as cancer can have very subtle and slow signs, especially early on. If a disease is discovered early on, the treatment is often easier and your pet’s chances to return to a normal life are better.
Even if your pet seems normal or is only showing some mild normal changes as he or she ages, there are several things that you can do to help keep them healthy and enhance their vitality.
Regular health examinations and wellness testing. Your pet should have a thorough physical examination at least once yearly. This may increase to twice yearly as your pet gets older or if he or she develops certain health concerns. Remember, pets age quicker than humans and a lot of things can happen in 6-12 months.
Wellness testing through blood and/or urine tests is an excellent way to detect health changes early on, when they are more treatable, and before your pet is feeling unwell. This is helpful throughout life but becomes more important as your pet ages. Any changes your pet has can be tracked over time.
Nutrition. Nutrition science has come a long way for both humans and pets. There are some truly excellent foods available to help support your pet’s healthy aging. They contain good quality proteins and carnitine to help maintain your pet’s muscle mass, a different nutritional profile to reduce the workload on the liver and kidneys, joint supplements to help support joint health and slow osteoarthritis, antioxidants and omega fatty acids to reduce free radical damage and decrease inflammation, which benefits every tissue in the body and helps with brain aging. Some senior foods also have special formulations to help with dental health or reduce the risk of bladder and kidney stones. We can recommend the best diet for your pet’s individual needs.
Supplements. The elixir of youth has not been discovered yet! But there are supplements that can be of benefit. Always ask your veterinarian before starting your pet on any supplements. Some examples of supplements that can help senior pets include: joint supplements, antioxidant vitamins E and C, omega fatty acids, probiotics, and SAMe which is helpful for liver and brain health.
Exercise and play. Your pet has always depended on you for the mental and physical stimulation of exercise, and this need does not go away when they age. Your cat may not be jumping up to the top of the fridge, and your dog may not be chasing Frisbees at the park, in fact these high-impact activities may be detrimental. Shorter but more frequent walks (dogs), or play sessions (cats), can still provide benefits for joints and muscles, as well as bonding and mental stimulation. Ask your veterinarian if you are unsure what type of exercise or play is best for your senior pet.
Tender Loving Care. Your senior pet is still a part of the family and has a lot of love to give. His or her needs will now be different than when he or she was a bouncy two-year-old. You may need to provide more grooming assistance, give medications, or provide help to get around. You may need to engage them in a different type of activity than before (romps at the dog park with Fido become quiet snuggles by the fireside, and running to chase a ball with Fifi becomes gentle swatting at a feather on a stick.) You may need to make changes like adding an extra litterbox on the main floor, placing steps up to the bed, or setting up your pet’s bed or perch near a window (cats) or near family activities (dog) so he or she can still enjoy life’s joys even with limited mobility.
Here’s a difficult topic, one that every pet owner thinks about and tries not to think about! Veterinarians are pet owners too, and we know how very hard this can be. Sometimes a pet will die on his or her own, suddenly or as expected, and this can be very hard in different ways. However, many times we have the responsibility and the opportunity to help ease our beloved pet’s passing into death when he or she is feeling unwell has no chance of recovery, or his or her quality of life is no longer sufficient and we have tried everything reasonable to no avail.
Dr. Alice Villalobos, the veterinarian who started Pawspice, a quality of life program for terminal pets, has published a scoring system for life quality called The HHHHHMM scale. The letters stand for: Hurt, Hunger, Hydration, Hygiene, Happiness, Mobility, and More Good Days than Bad. The scale is located at the end of the following article:
Euthanasia
Euthanasia is from the Greek euthanatos meaning ‘easy death’, though saying goodbye often seems impossible and not easy at all! We will guide you through the decision making process and help you through the last moments with your beloved pet. The procedure itself is through the injection of an anesthetic drug overdose, which is as peaceful and as painless as possible. You may like to stay with your pet to the end or say your goodbyes before this procedure. There are several options for the aftercare of your pet’s body, including burial, or cremation with or without the return of your pet’s ashes to you in an urn of your choice.
Grieving is a normal emotional response to a loss, and it is normal to go through many emotions after the loss of a pet, including sadness but also less expected ones like relief, anger and guilt. Allow yourself to experience these emotions and seek comfort in whatever ways you find helpful. If you or someone you know is having difficulty with their grieving process, there are resources to help, be it loved ones, a doctor, counselor, religious mentor, or the Ontario Veterinary College Pet Loss Support Hotline 519-824-4120 x53694 or email: petloss@uoguelph.ca.
Top 10 books to read with your children to help cope with pet loss